For decades, we’ve been told that winning the "war on cancer" depends on the next miracle drug or a high tech breakthrough in a laboratory. But a global analysis from early 2026 suggests we’ve been looking in the wrong direction. The most effective "cure" might not be a pill at all, but a fundamental change in how we live, work, and govern.
The Number That Changes Everything
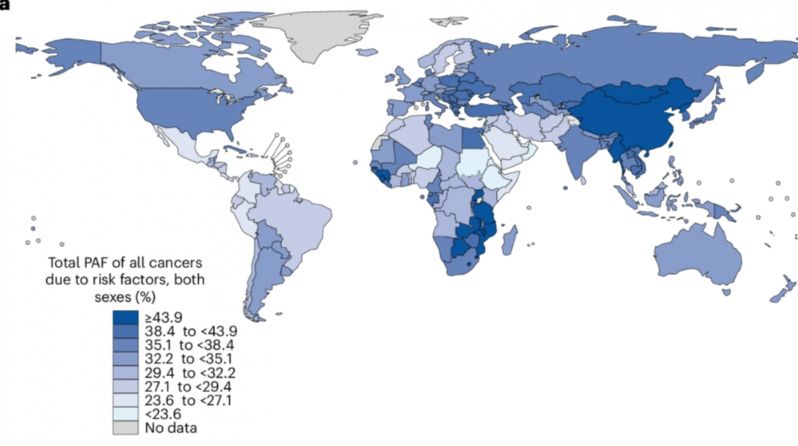
Researchers looking at data from nearly every country found a staggering statistic: nearly 4 out of every 10 new cancer cases are preventable. In 2022 alone, that represented over seven million diagnoses that didn't have to happen. These weren't just "bad luck" or "bad genes", they were cases linked to smoking, alcohol use, chronic infections, air pollution, and excess body weight. This reframes cancer entirely. It is not just a biological mystery; it is a social and political challenge that requires a collective response.
The Heavy Hitters: Smoking and Infections
If we want to dent the global cancer rate, we must start with the two biggest drivers: tobacco and microbes. Smoking remains the single largest cause of preventable death, accounting for roughly one in seven cancers globally. While we often talk about "willpower," history shows that cancer rates plummet most effectively when countries raise tobacco taxes and ban indoor smoking.
Similarly, many people are unaware that viruses and bacteria are potent carcinogens. HPV drives cervical cancer, Hepatitis fuels liver cancer, and H. pylori causes stomach cancer. We already possess the tools to stop these, including life-saving vaccines and basic screenings, yet they remain tragically underused in many parts of the world where healthcare infrastructure is thin.
Your Zip Code vs. Your Genetic Code
Not all cancer risks are a personal choice. You don’t choose to breathe polluted air or work in a factory with unsafe chemicals. Millions of people are exposed to fine particulate matter, asbestos, or benzene simply because of where they live or what they do for a living. This creates a form of environmental inequality, where your risk of cancer is often determined more by your postal code and local regulations than by your behavior. Reducing these risks isn't about "lifestyle tips"; it requires sustained regulation, enforcement, and a shift toward cleaner energy.
The Narrowing Gender Gap
Historically, men faced a much higher share of preventable cancer risk, largely due to higher rates of smoking and industrial exposures. However, that gap is closing. In many high-income countries, the rates of smoking and alcohol use among women have risen significantly. When combined with increasing rates of obesity and physical inactivity, we see a rise in breast, colorectal, and metabolic-linked cancers. This means our prevention strategies can no longer be "one size fits all", they must adapt to the changing ways that everyone lives today.
Why Treatment Alone Is Not Enough
Modern oncology has made incredible strides, and many once fatal cancers are now treatable. However, we cannot simply "treat" our way out of this crisis. With global cases expected to skyrocket by 2040, relying solely on expensive, complex medical interventions is like trying to empty the ocean with a teaspoon. It is economically and ethically unsustainable. Even the most perfect therapies cannot keep pace with a rising tide of preventable disease. Prevention is the only solution that actually scales.
What Prevention Really Means
In our culture, "prevention" is often reduced to individual advice like "eat your greens." While that matters, true prevention is a systemic effort. It means making tobacco and alcohol harder to market, ensuring every child has access to cancer-preventing vaccines, and cleaning the air we all breathe. It involves protecting workers from toxins and designing cities that make movement a natural part of daily life. These are collective choices that determine the health of millions.
A Different Way to Think About Cancer
Cancer is often shrouded in a sense of inevitability, a "lightning strike" of bad luck. While biology and genetics will always play a role, the data shows that millions of future diagnoses are already being written into today’s policies and environments. We don't have to wait for a lab breakthrough to save those lives; we just have to choose to act on what we already know. Whether these future cases come to pass is, to a surprising degree, up to us.
Reference
1. Fink H, Langselius O, Vignat J, et al. Global and regional cancer burden attributable to modifiable risk factors to inform prevention. Nat Med. Published online February 3, 2026. doi:10.1038/s41591-026-04219-7
2. Wild CP, Weiderpass E, Stewart BW, eds. World Cancer Report: Cancer research for cancer prevention. Lyon (FR): International Agency for Research on Cancer; 2020.
3. Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71(3):209-249. doi:10.3322/caac.21660
4. Islami F, Goding Sauer A, Miller KD, et al. Proportion and number of cancer cases and deaths attributable to potentially modifiable risk factors in the United States. CA Cancer J Clin. 2018;68(1):31-54. doi:10.3322/caac.21440
5. World Health Organization. WHO report on the global tobacco epidemic, 2023: protect people from tobacco smoke. Geneva, Switzerland: World Health Organization; 2023.